In challenging, dangerous and life-threatening situations, first responders are usually the first ones on the scene. Not only do they are the first ones to reach out to disaster survivors and save lives, but they also provide physical and emotional support. In Australia, community first responders are volunteers with basic skills for responding to medical emergencies.
Whether you are in the emergency healthcare services, a community first responder or a cautious parent taking your kids on a winter adventure, when it comes to first aid kits, “better safe than sorry” is the biggest understatement of the year.

What Should a Trauma Kit Contain?
Tourniquet
Despite some controversies about the long-term outcomes of its use, it has been established that proper tourniquet use can save lives. In an emergency or military setting, there may be neither time nor resources to control hemorrhage. Additionally, it’s rarely possible to extract injured people from danger while continuously applying pressure by hand or keeping an injured limb elevated, especially in the case of multiple casualties. That’s where emergency tourniquets come in.
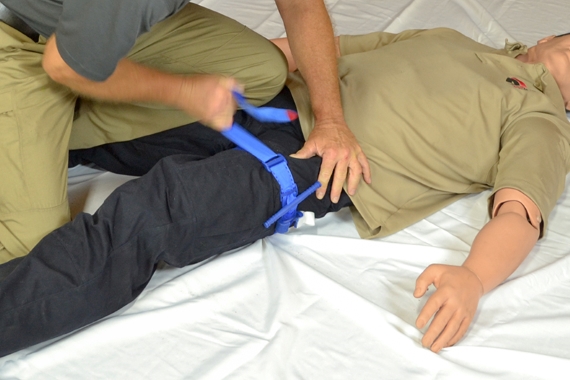
The clinical risk of possible ischemic complications is topped by its lifesaving capacity. Medical organizations advise that both medical and nonmedical personnel be competent in tourniquet use as an early application of tourniquets has reduced death rates. Severe hemorrhage may not continue when an effective tourniquet is released after 2 hours.
It should only be applied if the hemorrhage is life-threatening, all conventional measures have failed and the consequences of applying a tourniquet can be managed appropriately. The risks of ischemic complications and hemorrhage are minimal within a 2-hour use. Beyond 6 hours, the risk of arrhythmias and crush syndrome is so high that amputation above the level of the tourniquet is mandatory. It should be simultaneously broad and tight enough, positioned as low as possible but never over a joint. Narrow, improvised tourniquets should be removed or replaced as soon as possible.
At the end of 2013, the Israel Defense Force Medical Corps (IDF-MC) introduced the Combat Application Tourniquet (CAT) to all units as a standard item for first-aid use. The aim was to replace the silicone and “Russian” tourniquets due to the high failure rates of lower limb hemorrhage control and the superiority of CAT. They haven’t been used since 2016.
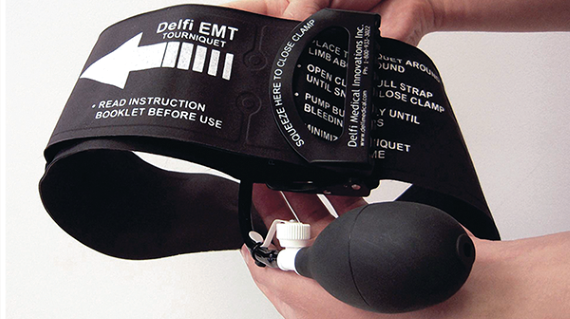
The CAT (Combat Application Tourniquet) is a small and lightweight arterial tourniquet used for controlling life-threatening bleeding. Its one-handed windlass system, self-adhering band and friction adaptor buckle allow complete occlusion of blood flow in extremities of different sizes. The IDF-MC also performed an analysis based on their extensive database comparing hospital amputation before and after CAT use. The rate was similar, confirming the safety of the tourniquet in contrast to the fear of the increased risk of amputations.
The authors recommended sticking to direct pressure in the prehospital setting only when medical personnel judged the tourniquet as unnecessary and when evacuation time is estimated to be longer than an hour and if the injury is not older than 2 hours. In case the provider is a physician or a paramedic, time from injury extends to six hours.

The casualties with an applied tourniquet also had a lower heart rate and a higher systolic blood pressure upon arrival to the emergency department, a shorter median length of stay and a lower rate of hospitalizations of 7 days. Civilian tourniquet training programs are based on military programs and the CAT is widely used by civilian organizations.
Nitrile Gloves
In addition to the rise of latex allergies, the durability and resistance to chemicals are reasons why nitrile gloves are better than latex gloves. These gloves are the perfect choice for anyone who has to handle potentially hazardous and corrosive chemicals. They’re also suited for most medical environments, being puncture and biohazard resistant. In hazardous situations, choosing the right gloves will increase productivity and functionality while reducing risks for end-users and patients.

Emergency Bandage
Just like a bandage used for immobilizing sprained ankles, knees, wrists and elbows, the emergency (Israeli) bandage is an elastic one. However, it has been optimized in 3 aspects: the dressing, the pressure and the closure bar.
The dressing is a sterile (vacuum-packed) nonadherent dressing and its removal is easily done without reopening the wound. The pressure bar increases tightness and pressure beneath it while the closure bar (placed above the pressure bar) can secure the bandage with a one-handed sliding motion. Moreover, the closure bar can be used to create additional pressure by its sliding under a surface dressing layer and twisting the bandage wrapping.
The emergency bandage can place much higher pressure on the bleeding site while producing a tourniquet-like effect at the bleeding site, raising hemorrhage control to the next level. Its superiority is what makes it adequate for traffic accidents, workplace accidents, home injuries, gunshot wounds, stab and other assault wounds.

Bite Bandage
Around 5.4 million people are bitten by snakes while 81000 to 138000 people die every year from snake bites. The number of amputations and permanent disabilities are three times higher. In Queensland, there were 872 snake bites last year while 30 bites were reported in the first 22 days of 2021. 9 in 10 bites have happened in people’s homes or yards.
Agricultural workers and children are at the biggest risk. Even if you don’t live in an area where snakes are common, it’s always useful to know what is the first aid treatment for a snake bite. The right snake bite bandage is designed for the Pressure Immobilisation Technique (PIT), used for the treatment of all Australian Snake and Funnel Webbed Spider bites, Blue Ringed Octopus and Cone Shell sting.
They are much wider and longer than most regular elastic bandages, with the ability to fully bandage an adult leg. The unique stitching technology ensures the even application of correct pressure to the entire limb. These characteristics are crucial for the effective treatment of snakebite. Although it will definitely come in handy wherever you are, a snake bite bandage is a must-have item in a remote or wilderness first aid kit.
Chest Seal
A chest seal is a lifesaver when it comes to penetrating chest trauma. Its vented channels allow air to escape the chest cavity during exhalation while preventing it to enter during inhalation. Consequently, this reduces the risk of life-threatening pneumothorax. The proper chest seal has a superior adhesive that can stick to sweaty, bloody or hairy patients. Packaged in a rugged, easy-to-open foil pouch, Its compact and perforated packaging allows users to pack it with no trouble and open only one dressing at a time when needed.

Without a doubt, proper application is key to success. Although there must be advantages to the online courses you’ve been taking, there’s nothing like the experience of training. A chest seal trainer is a cost-effective, premium training alternative for both vented and occlusive chest seals. It’s specifically designed to look like the real deal in order to accommodate and familiarise the user.
Universal Shears
Small universal shears, as their name says, can be used on numerous occasions. They are mostly used in first aid situations due to their small size and effectiveness in trimming not only bandages, medical tapes and adhesive dressings but also fabrics and plastic. This would mean that you can use them to remove clothing, open packages and trimming or removing adhesive tapes. No first aid kit should come without a pair of universal shears. It’s always smart to keep a spare.
Emergency Thermal Blanket
Hypothermia is a decrease in core body temperature below 35°C. Fatal hypothermia occurs at body temperatures of 26°C to 29°C. Hypothermia can be induced by physical conditions or by trauma and shock. Believe it or not, Australia’s death rate due to cold weather is 6.5%, almost double than Sweden. This is assumed to be due to the low quality of housing.

On the other hand, hypothermia treatment is crucial when providing first aid to trauma-induced shock, when the body is incapable of maintaining sufficient body temperature. Thermal blankets made with ReflexcellTM technology have been proven to have higher thermal resistance while remaining compact and lightweight. Hence, a foil blanket to reflect body heat and prevent shock can be included even in the smallest of first aid kits.


